急性呼吸窘迫综合征(acute respiratory distress syndrome ARDS)是由肺内外多种因素(如肺炎、脓毒症、严重创伤、吸入)引起的一种复杂的临床疾病。尽管我们对ARDS有着深刻的认知,但其临床病死率仍较高,ARDS的全球总体病死率仍波动在30%~46%[1],其中轻、中、重度患者的病死率分别为34.9%、40.3%和46.1%[2-3],临床治疗面临着巨大挑战,1960-1990年治疗以高潮气量通气为主,但发现呼吸机相关肺损伤(ventilator associated lung injury VILI)会给患者带来严重并发症,开始推动保护性通气策略(小潮气量、限制平台压),至2000年,俯卧位通气(prone position ventilation PPV)治疗逐渐被运用于ARDS成人患者中,根据临床观察以及理论分析,PPV似乎是一种有效改善预后且经济适用的临床治疗手段。2020年COVID-19大流行期间,WHO紧急指南强烈建议将俯卧位作为重症COVID-19 ARDS的一线干预[3-5]。然而,PPV仍面临挑战:约20%患者存在“无反应性”[6-7],总结其原因可能是:肺实质病变的不可逆性、患者个体差异性、治疗时间与周期不确定性,经2018年《新英格兰医学杂志》发表的PROSEVA试验的首次证实,对中重度ARDS患者早期实施每日超过16 h的PPV,可使28 d病死率从32.8%显著降至16.0%[8-10],这也是最早针对俯卧位维持时间的研究,经过2019-2024年大量临床治疗经验的总结,提出长程俯卧位通气(prolonged prone position ventilation PPPV)概念。PPPV指在急性呼吸窘迫综合征(ARDS)患者中,治疗上通常以单次俯卧位持续时间≥24 h、多疗程肺保护性通气为特点,其核心目标为通过持续的重力依赖性肺复张改善顽固性低氧血症及降低呼吸机相关性肺损伤风险[3, 10]。在COVID-19大流行期间,PPPV实现了突破性革新,PPPV被常规化,俯卧位应被视为保护性通气策略的核心组成部分,应当延长俯卧位治疗时间窗,而非反复短时翻转[9, 11-13]。COVID-19 ARDS患者俯卧位反应个体差异大,常因弥漫性病变导致整体通气血流匹配改善不显著,约2/3患者早期氧合无改善,而非COVID ARDS反应更一致[14]。但匹配基线氧合与顺应性后,两组生理反应差异无统计学意义,提示COVID-19患者同样可获益[10]。
2 长程俯卧位通气 2.1 病理生理仰卧位时,重力梯度、心脏压迫及腹腔高压共同导致背侧依赖区胸膜腔内压显著升高,跨肺压降低诱发肺泡塌陷;同时腹侧非依赖区跨肺压过度增高易诱发区域性过度膨胀[15-21]。俯卧位时,重力方向逆转使背侧,胸腔负压增大,跨肺压升高促进肺泡复张,而腹侧胸腔负压减小致跨肺压降低,有效减轻过度膨胀,全肺复张体积显著提升。此种跨肺压梯度均等优化了通气/灌注匹配,构成氧合改善的生理基础,长程俯卧位通气特点是持续扩大这种生理优势[17, 20, 22]。在进行长程俯卧位通气治疗时,往往需要充分的镇痛镇静,甚至予以肌松,镇静状态所致膈肌张力降低时,体位改变降低腹腔内压,促使膈肌尾向移位,解除腹腔内容物对背侧肺基底区的压迫,以此更加有利于气血交换。
实施长程俯卧位后,背侧肺泡复张使得区域性通气改善,同时肺血流分布趋向均匀化,促使肺内分流率下降21%~50%[17],俯卧位时依赖区灌注相对增加而通气适度减少,使生理死腔量下降20%~47%[15-17];值得注意的是,Gattinoni等[23]发现俯卧位后二氧化碳分压降低超过1 mmHg与病死率改善显著相关,提示死腔减少可能通过改善肺血管功能影响预后,更深层的机制涉及通气血流双重均质化——俯卧位不仅通过跨肺压梯度逆转使通气分布更均一,长程俯卧位更通过削弱重力对血流分布的主导作用,实现全肺血流分布优化[16];Nyren等[24]证实俯卧位时腹侧重力依赖区并未形成灌注优势,此种通气血流的同步均质化构成V/Q匹配改善的病理生理基础,这种优势可以总结为原本受压的背侧肺泡毛细血管复张,血流重新分布,减轻了腹侧区域毛细血管的过度灌注与剪切应力,这使得红细胞在肺毛细血管网络中接触肺泡壁的空间更均一[4, 17, 20, 25-26],均匀的血流灌注提升了肺泡上皮细胞氧气交换效率,并减轻了局部血管内皮因血流冲击或缺血再灌注所引发的炎症反应与损伤,从而改善氧合,保护微血管功能;长程俯卧位通气亦可降低呼吸机相关性肺损伤(ventilator-induced lung injury VILI)。影像学检查可证实俯卧位时全肺复张体积增加6.0%,肺不张指数从1.41%降至1.30%,直观反映肺可复张性改善,顺应性提升——相同潮气量下驱动压显著下降(EIT监测显示平均降幅3~5 cmH2O)[16]。更深层的肺保护效应体现在VILI三维防控:①气压伤预防:通气均质化消除局部应力集中,允许安全降低PEEP水平(较仰卧位降低3~5 cmH2O)[4, 16, 27];②剪切伤减少:依赖区肺泡稳定开放避免呼气末塌陷/吸气初复张循环,显著降低界面剪切力[3, 16, 19, 27-30]。③生物创伤抑制:机械应力降低,抑制炎症因子(TNF-α、IL-6、IL-8)释放,动物模型证实俯卧位可减轻肺组织凋亡及远端器官损伤,Papazian等[26]发现俯卧位后支气管肺泡灌洗液IL-8水平下降,随着时间推移,这种优势表现出轻微增强;除呼吸力学优化外,长程俯卧位通气对循环系统产生多重调节效应:长程俯卧位通气通过促进肺泡复张、改善氧合,有效缓解低氧性肺血管收缩(HPV),持续降低肺动脉压与肺血管阻力(PVR),从而显著减轻右心室后负荷[9]。这一机制可减少右心室扩张与室间隔运动障碍,对合并急性肺源性心脏病(ACP)的ARDS患者具有重要治疗意义。心输出量总体维持稳定或轻度上升,其变化取决于患者容量状态及心功能基础。同时,左心室功能亦获改善,一方面源于右心室后负荷降低减轻室间隔左移、优化左心室充盈,另一方面得益于氧输送提升改善心肌氧供,尤其有益于心功能不全患者[1, 3-4, 31]。
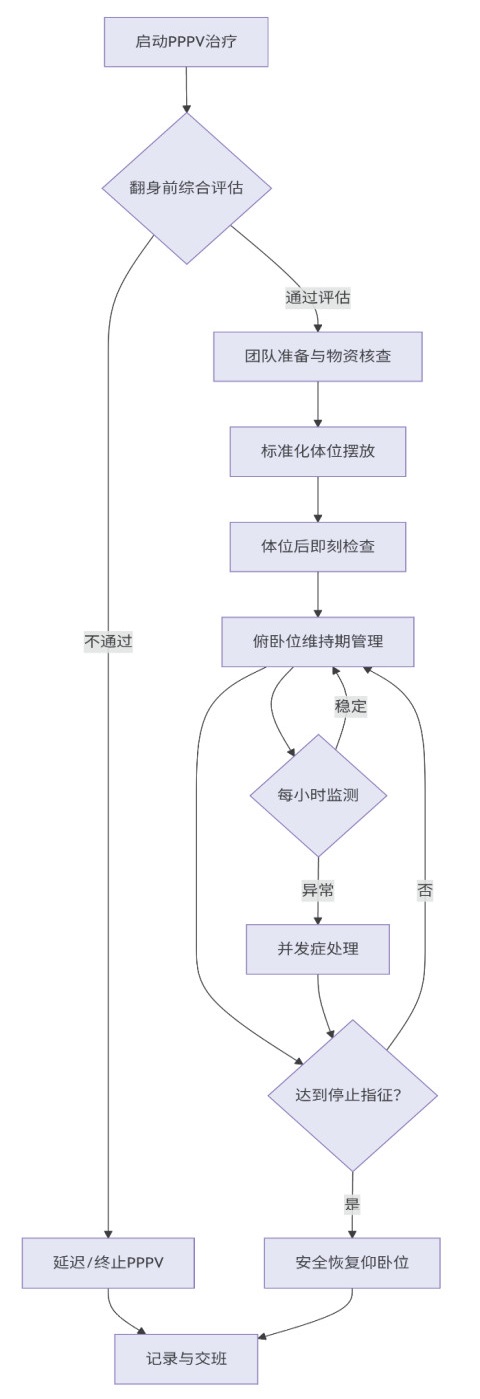
2.2 临床实践长程俯卧位通气(PPPV)的实施需多团队标准化协作。建议由4~5名训练有素人员共同执行,备齐专用枕垫、防压疮材料及急救设备。首先进行深度镇静镇痛,必要时使用肌松剂,妥善固定气道及各类管路,预吸痰并暂停肠内营养。翻身时需专人指挥,统一行动,采用轴向翻身法将患者转为俯卧位。体位安置时,头部置于专用软枕并偏向一侧,定期更换方向;胸廓、骨盆及下肢需垫软枕支撑,保持腹部悬空,以减轻膈肌压迫。同时需严密保护骨突处皮肤及双眼。每日暂停1次评估神经功能及并发症(压疮、角膜损伤等),俯卧位持续时间超过24 h,每次翻身前行内环境及血气监测。长程俯卧位实施流程图见图 1。
|
| 图 1 长程俯卧位实施流程图 |
|
|
有研究表明:针对清醒患者,长程俯卧位通气可使其氧合指数显著改善,且该改善效应在患者恢复仰卧位后仍持续存在[32-33]。并且从病理生理学视角看,在某些插管的ARDS患者中,俯卧位带来的有益生理效应(静态与动态顺应性增加)可持续16 h,且在恢复仰卧位后至少维持24 h [12],此种效果得益于患者俯卧位后可能激活了相似的病理生理机制。Brugliera等[34]发现针对ARDS患者,单次俯卧位持续时间中位数为30 h,可以显著改善氧合且未增加并发症。Okin等[13]认为对COVID-19插管患者采用PPPV治疗具有多重潜在优势:(1)呼吸系统顺应性改善以及肺应变降低的优势在俯卧位后24 h持续增强,且每日PPV持续时间超过12 h且患者接受低潮气量通气(LTVV;≤8 mL/kg),PPPV治疗能够有效降低病死率。(2)反复改变体位可能导致肺萎陷加重以及VILI加重,从而可能增加病死率[32, 35]。原因可能是反复体位转换会中断肺复张的维持,导致肺泡周期性开闭,这种机械应力会产生剪切力损伤肺组织,加重肺不张和加剧呼吸机相关肺损伤,进而引发炎症反应,最终导致器官功能负担增加[36]。然而,Karlis等[9]认为与间歇俯卧通气策略相比,长程俯卧位方案在改善氧合和呼吸力学方面没有任何优势,但其研究中28 d病死率与Okin研究高度接近(PPPV组21.6% vs. 25.5%;SPPV组34.6% vs. 34.9%),两者都认同这一观点:针对ARDS患者,体位翻转越频繁,病死率越高。主要结果的差异可能来源于Karlis的研究是一项样本量小、单中心非随机研究,可能存在选择偏倚风险[9]。尽管延长俯卧位通气(PPPV)在改善氧合与降低病死率方面具有显著优势,但其临床疗效仍存在个体差异性。因此,及时评估患者对PPPV的治疗反应,并精准区分反应者与无反应者,成为优化治疗策略的关键环节。俯卧位通气时床面对胸廓前壁及腹壁的扩张产生限制,导致胸壁顺应性下降;相反,当患者转为仰卧位时,肺顺应性和呼吸系统顺应性则会增加[37]。Langer等[38]观察到俯卧位后呼吸频率设置显著增加,且分钟通气量有升高趋势。因此,需通过通气比率(ventilatory ratio)的变化来区分CO2应答与非应答者,从而反映死腔的变化。也有研究认为监测PaCO2的变化在预测ARDS患者对俯卧位PPPV的反应方面,可能比监测P/F比值的变化更相关[39]。这方面仍需前瞻性多中心随机对照试验验证生物标志物的预测价值、结合电阻抗断层成像(EIT)实时监测区域性肺通气、建立机器学习模型整合多参数动态预测疗效;长期随访评估神经肌肉并发症等远期结局[9, 35, 41-42]。EIT通过实时监测将长程俯卧位从经验转向精准:VTdep(背侧潮气通气百分比)快速下降提示去复张需继续;若VTdep稳定且塌陷/膨胀平衡、GI指数改善,提示肺泡复张维持,可安全终止[43-44]。
2.3 无反应性患者(1)Dell' Anna等[45]研究提示,俯卧位改善氧合的作用可能独立于传统PEEP诱导的肺可复张性,部分患者因肺实质病变进入纤维增生期、重力依赖性肺水肿轻微或胸壁顺应性严重下降,导致塌陷肺泡复张受限,即使实施俯卧位也无法实现有效肺复张。因此,通过影像学(如CT定量评估可复张肺体积)或功能性监测(如EIT动态观察背侧通气变化)识别肺可复张性低下的患者,有助于早期预判无反应风险并调整治疗策略;(2)ARDS表型异质性显著影响俯卧位反应:局部型患者俯卧位3 h内氧合迅速改善,而非局部型患者需6 h方显效,常规疗程易误判为无反应;高D-二聚体患者因肺血管微血栓及内皮损伤,通气血流匹配优化延迟。基于影像学表型与生物标志物识别反应延迟者,实施个体化长程俯卧位,可避免无效治疗并改善预后[19]。
3 并发症 3.1 压力性损伤(pressure injury,PI)长程俯卧位通气最常见的并发症之一是压力性损伤(pressure injury,PI)。由于身体局部长时间受压,特别是骨骼突起部位(如髂前上棘、膝盖)和面部(如颧骨、下颌部),会影响局部血液循环,导致皮肤及皮下组织损伤。首先通过分层风险评估工具(如Braden量表及Munro量表)识别高危患者(Braden≤12分或Munro≥40分),此类患者皮肤更容易损伤[9, 46-47]。其次,实施标准化体位管理,包括使用硅胶减压垫保护骨突部位(颧骨、下颌)、动态调整头部方向(每2 h侧倾15°~30°),并采用交替充气床垫联合实时压力监测系统以降低局部受压强度(目标压力 < 32 mmHg);皮肤护理方面,预防性应用透明薄膜敷料或硅胶泡沫敷料覆盖高风险区域;全身状态优化需保证充足营养支持[热量25~30 kcal/(kg·d)、蛋白质1.5~2.5 g/(kg·d)]及微循环稳定(MAP≥65 mmHg,血乳酸<2 mmol/L);通过上述综合措施,可将ICU患者PI发生率降至15%以下[41, 48-50]。
3.2 反流在重度ARDS患者进行长程俯卧位治疗时,进行肠内营养(EN)被认为可行的[51],通常选择减量胃管肠内营养,但也有可能导致患者严重的营养不良,特别是分解代谢水平高的疾病期间[52],这就需要采用高热量密度肠内营养配方进行24 h连续喂养,以减少每小时输注量,而保证每日热量[31, 40, 51, 53]。使用胃管内营养,反流和误吸发生率高达88.9%[32]。幽门后喂养可显著降低反流与误吸风险[54],减少呼吸机相关性肺炎,且体位翻转时无需中断输注,保障热量达标[55]。但需配套置管技术、床头抬高及促动力药物等综合防控策略,确保安全。在进行俯卧位前,评估胃残余量(GRV):若GRV>250~300 mL,应考虑延迟翻身或调整喂养策略,以低速开始(如20~25 mL/h)喂养,每4~6 h监测,对于存在胃轻瘫或GRV增高的患者,可尝试予以促胃肠动力药物。但是也有研究提出单独GRV指标特异性不高,应结合其他临床表现(如呕吐、腹胀)综合判断。
3.3 神经丛病变长期并发症主要是神经丛病,特别是臂丛麻痹,其他长期并发症包括周围神经损伤,特别是腓神经麻痹、股外侧皮神经损伤。首先遵循标准化体位摆放流程,采用双臂内收体位,避免臂丛神经过度牵拉或受压[34];下肢采用膝关节屈曲15°~20°并垫高踝部,降低腓总神经卡压风险;动态监测方面,通过体感诱发电位或高频超声评估神经束膜水肿[56],联合每日四肢感觉运动功能评估;高危患者(如糖尿病性周围神经病变或BMI>30 kg/m2)推荐使用神经保护装置, 如硅胶分指垫隔离尺神经沟,并限制镇静深度以保留自主体位调节能力[9, 46, 57-58]。
长程俯卧位通气作为ARDS肺保护性通气策略的核心组成部分,EIT监测为实施PPPV提供了重要的生理学依据。然而,目前基于常规临床参数的机器学习模型预测效果不佳,传统以早期氧合定义反应者低估远期获益。当前研究的主要瓶颈在于缺乏一套能够整合EIT实时动态数据、多维度生物标志物以及动态预测算法的精准分型系统。未来研究应致力于构建“监测-预测-干预”一体化闭环:通过开发集成V/Q力学的多模态EIT平台,结合深度学习构建动态校准预测模型,积极开展RCT验证临床价值,最终建立从急性期生理优化到远期预后改善的完整循证体系。
利益冲突 所有作者声明无利益冲突
| [1] | Al-Husinat L, Azzam S, Al Sharie S, et al. A narrative review on the future of ARDS: evolving definitions, pathophysiology, and tailored management[J]. Crit Care, 2025, 29(1): 88. DOI:10.1186/s13054-025-05291-0 |
| [2] | Bellani G, Laffey JG, Pham T, et al. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries[J]. Jama, 2016, 315(8): 788. DOI:10.1001/jama.2016.0291 |
| [3] | Cave C, Samano D, Sharma AM, et al. Acute respiratory distress syndrome: a review of ARDS across the life course[J]. J Investig Med, 2024, 72(8): 798-818. DOI:10.1177/10815589241270612 |
| [4] | Fossali T, Pavlovsky B, Ottolina D, et al. Effects of prone position on lung recruitment and ventilation-perfusion matching in patients with COVID-19 acute respiratory distress syndrome: a combined CT scan/electrical impedance tomography study[J]. Crit Care Med, 2022, 50(5): 723-732. DOI:10.1097/ccm.0000000000005450 |
| [5] | Majumder J, Minko T. Recent developments on therapeutic and diagnostic approaches for COVID-19[J]. AAPS J, 2021, 23(1): 14. DOI:10.1208/s12248-020-00532-2 |
| [6] | Ochani R, Asad A, Yasmin F, Shaikh S, Khalid H, Batra S, Sohail MR, Mahmood SF, Ochani R, Hussham Arshad M, et al. COVID-19 pandemic: from origins to outcomes. A comprehensive review of viral pathogenesis, clinical manifestations, diagnostic evaluation, and management[J]. Infez Med, 2021, 29(1): 20-36. |
| [7] | Shelhamer M, Baxi S, Wesson P, et al. Response to prone vs. supine ventilation and mortality outcome in intubated COVID-19 patients[J]. J Intensive Care Med, 2023, 38(3): 322. DOI:10.1177/08850666221147226 |
| [8] | Guérin C, Reignier J, Richard JC, et al. Prone positioning in severe acute respiratory distress syndrome[J]. N Engl J Med, 2013, 368(23): 2159-2168. DOI:10.1056/nejmoa1214103 |
| [9] | Karlis G, Markantonaki D, Kakavas S, et al. Prone position ventilation in severe ARDS due to COVID-19: comparison between prolonged and intermittent strategies[J]. J Clin Med, 2023, 12(10): 3526. DOI:10.3390/jcm12103526 |
| [10] | Park J, Lee HY, Lee J, et al. Effect of prone positioning on oxygenation and static respiratory system compliance in COVID-19 ARDS vs. non-COVID ARDS[J]. Respir Res, 2021, 22(1): 220. DOI:10.1186/s12931-021-01819-4 |
| [11] | Jochmans S, Mazerand S, Chelly J, et al. Duration of prone position sessions: a prospective cohort study[J]. Ann Intensive Care, 2020, 10: 66. DOI:10.1186/s13613-020-00683-7 |
| [12] | Page DB, Vijaykumar K, Russell DW, et al. Prolonged prone positioning for COVID-19–induced acute respiratory distress syndrome: a randomized pilot clinical trial[J]. Ann Am Thorac Soc, 2022, 19(4): 685-687. DOI:10.1513/annalsats.202104-498rl |
| [13] | Okin D, Huang CY, Alba GA, et al. Prolonged prone position ventilation is associated with reduced mortality in intubated COVID-19 patients[J]. Chest, 2023, 163(3): 533-542. DOI:10.1016/j.chest.2022.10.034 |
| [14] | Yang YY, Li HT, Chi Y, et al. Ventilation-perfusion matching in early-stage of prone position ventilation: a prospective cohort study between COVID-19 ARDS and ARDS from other etiologies[J]. Physiol Meas, 2025, 46(1): 015007. DOI:10.1088/1361-6579/ada8f1 |
| [15] | Li YF, Hu QQ, Wang WJ, et al. Development of prone position ventilation device and study on the application effect of combined life support technology in critically ill patients[J]. Can Respir J, 2024, 2024: 5812829. DOI:10.1155/2024/5812829 |
| [16] | Liao XY, Meng L, Zeng ZY. Prone position ventilation for the relief of acute respiratory distress syndrome through improved pulmonary ventilation: Efficacy and safety[J]. Nurs Crit Care, 2024, 29(2): 255-273. DOI:10.1111/nicc.12948 |
| [17] | Sud S, Fan E, Adhikari NKJ, et al. Comparison of venovenous extracorporeal membrane oxygenation, prone position and supine mechanical ventilation for severely hypoxemic acute respiratory distress syndrome: a network meta-analysis[J]. Intensive Care Med, 2024, 50(7): 1021-1034. DOI:10.1007/s00134-024-07492-7 |
| [18] | Wang YX, Song JQ, Lin SY, et al. Influence of prone position on regional ventilation/perfusion matching in patients with ARDS over time[J]. Respir Care, 2025, 70(7): 821-829. DOI:10.1089/respcare.12247 |
| [19] | Yang SH, Sun Q, Yuan XY, et al. Effect of prone position on ventilation-perfusion matching in patients with moderate to severe ARDS with different clinical phenotypes[J]. Respir Res, 2025, 26(1): 70. DOI:10.1186/s12931-025-03154-4 |
| [20] | Qin W, Mao L, Shen Y, et al. Prone position in the mechanical ventilation of acute respiratory distress syndrome children: a systematic review and meta-analysis[J]. Front Pediatr, 2024, 12: 1293453. DOI:10.3389/fped.2024.1293453 |
| [21] | Jørgensen VL, Adelsten J, Christensen S, et al. The use of prone position ventilation in Danish patients with COVID-19-induced severe acute respiratory distress syndrome treated with veno-venous extracorporeal membrane oxygenation: a nationwide cohort study with focus on pulmonary effects[J]. Acta Anaesthesiol Scand, 2024, 68(9): 1223-1233. DOI:10.1111/aas.14481 |
| [22] | Wright JM, Gerges C, Shammassian B, et al. Prone position ventilation in neurologically ill patients: a systematic review and proposed protocol[J]. Crit Care Med, 2021, 49(3): e269-e278. DOI:10.1097/ccm.0000000000004820 |
| [23] | Gattinoni L, Busana M, Giosa L, et al. Prone positioning in acute respiratory distress syndrome[J]. Semin Respir Crit Care Med, 2019, 40(1): 94-100. DOI:10.1055/s-0039-1685180 |
| [24] | Nyrén S, Mure M, Jacobsson H, et al. Pulmonary perfusion is more uniform in the prone than in the supine position: scintigraphy in healthy humans[J]. J Appl Physiol, 1999, 86(4): 1135-1141. DOI:10.1152/jappl.1999.86.4.1135 |
| [25] | Chao YL, Yuan XY, Zhao ZQ, et al. Physiologic effects of prone positioning on gas exchange and ventilation-perfusion matching in awake patients with AHRF[J]. BMC Pulm Med, 2024, 24(1): 600. DOI:10.1186/s12890-024-03411-0 |
| [26] | Papazian L, Munshi L, Guérin C. Prone position in mechanically ventilated patients[J]. Intensive Care Med, 2022, 48(8): 1062-1065. DOI:10.1007/s00134-022-06731-z |
| [27] | Vieillard-Baron A, Boissier F, Pesenti A. Hemodynamic impact of prone position. Let's protect the lung and its circulation to improve prognosis[J]. Intensive Care Med, 2023, 49(6): 692-694. DOI:10.1007/s00134-023-07001-2 |
| [28] | Guervilly C, Fournier T, Chommeloux J, et al. Ultra-lung-protective ventilation and biotrauma in severe ARDS patients on veno-venous extracorporeal membrane oxygenation: a randomized controlled study[J]. Crit Care, 2022, 26(1): 383. DOI:10.1186/s13054-022-04272-x |
| [29] | Niikawa H, Okamoto T, Ayyat KS, et al. Prone ex vivo lung perfusion protects human lungs from reperfusion injury[J]. Artif Organs, 2022, 46(11): 2226-2233. DOI:10.1111/aor.14328 |
| [30] | Walter T, Ricard JD. Extended prone positioning for intubated ARDS: a review[J]. Crit Care, 2023, 27(1): 264. DOI:10.1186/s13054-023-04526-2 |
| [31] | Liu CJ, Jiang JX, Wen ZJ, et al. Naso-intestinal versus gastric tube for enteral nutrition in patients undergoing mechanical ventilation: a systematic review and meta-analysis[J]. Syst Rev, 2025, 14(1): 13. DOI:10.1186/s13643-024-02743-6 |
| [32] | Ehrmann S, Li J, Ibarra-Estrada M, Perez Y, Pavlov I, McNicholas B, Roca O, Mirza S, Vines D, Garcia-Salcido R et al. |
| [33] | Liu L, Sun Q, Zhao HS, et al. Prolonged vs shorter awake prone positioning for COVID-19 patients with acute respiratory failure: a multicenter, randomised controlled trial[J]. Intensive Care Med, 2024, 50(8): 1298-1309. DOI:10.1007/s00134-024-07545-x |
| [34] | Brugliera L, Filippi M, Del Carro U, et al. Nerve compression injuries after prolonged prone position ventilation in patients with SARS-CoV-2: a case series[J]. Arch Phys Med Rehabil, 2021, 102(3): 359-362. DOI:10.1016/j.apmr.2020.10.131 |
| [35] | Boesing C, Graf PT, Schmitt F, et al. Effects of different positive end-expiratory pressure titration strategies during prone positioning in patients with acute respiratory distress syndrome: a prospective interventional study[J]. Crit Care, 2022, 26(1): 82. DOI:10.1186/s13054-022-03956-8 |
| [36] | Elmer N, Reißhauer A, Brehm K, et al. Long-term complications of prone position ventilation with relevance for acute and postacute rehabilitation: a systematic review of the literature[J]. Eur J Phys Rehabil Med, 2023, 59(1): 111-121. DOI:10.23736/s1973-9087.22.07529-3 |
| [37] | Guérin C, Albert RK, Beitler J, et al. Prone position in ARDS patients: why, when, how and for whom[J]. Intensive Care Med, 2020, 46(12): 2385-2396. DOI:10.1007/s00134-020-06306-w |
| [38] | Langer T, Brioni M, Guzzardella A, et al. Prone position in intubated, mechanically ventilated patients with COVID-19: a multi-centric study of more than 1000 patients[J]. Crit Care, 2021, 25(1): 128. DOI:10.1186/s13054-021-03552-2 |
| [39] | Liang HW, Deng QX, Ye WY, et al. Prone position ventilation-induced oxygenation improvement as a valuable predictor of survival in patients with acute respiratory distress syndrome: a retrospective observational study[J]. BMC Pulm Med, 2024, 24(1): 575. DOI:10.1186/s12890-024-03349-3 |
| [40] | Zagales R, Lee P, Kumar S, et al. Optimizing management of acute respiratory distress syndrome in critically ill surgical patients: a systematic review[J]. J Surg Res, 2025, 305: 385-397. DOI:10.1016/j.jss.2024.10.039 |
| [41] | Chen PH, Lee CH, Yen WT, et al. Efficacy and safety of prone positioning in patients undergoing extracorporeal membrane oxygenation (ECMO): a systematic review and meta-analysis[J]. J Clin Anesth, 2025, 103: 111786. DOI:10.1016/j.jclinane.2025.111786 |
| [42] | Franchineau G, Jonkman AH, Piquilloud L, et al. Electrical impedance tomography to monitor hypoxemic respiratory failure[J]. Am J Respir Crit Care Med, 2024, 209(6): 670-682. DOI:10.1164/rccm.202306-1118ci |
| [43] | Songsangvorn N, Xu YH, Lu C, et al. Electrical impedance tomography-guided positive end-expiratory pressure titration in ARDS: a systematic review and meta-analysis[J]. Intensive Care Med, 2024, 50(5): 617-631. DOI:10.1007/s00134-024-07362-2 |
| [44] | Nakamura H, Hirai T, Kurosawa H, et al. Current advances in pulmonary functional imaging[J]. Respir Investig, 2024, 62(1): 49-65. DOI:10.1016/j.resinv.2023.09.004 |
| [45] | Dell'Anna AM, Carelli S, Cicetti M, et al. Hemodynamic response to positive end-expiratory pressure and prone position in COVID-19 ARDS[J]. Respir Physiol Neurobiol, 2022, 298: 103844. DOI:10.1016/j.resp.2022.103844 |
| [46] | Makarawate P, Chimtim K, Mitsungnern T, et al. Comparison of standard and prone-position electrocardiograms in COVID-19 patients with pulmonary complications: correlations and implications[J]. Clin Cardiol, 2024, 47(10): e70024. DOI:10.1002/clc.70024 |
| [47] | Demir U, Taşkın Ö, Yılmaz A, et al. Does prolonged prone position affect intracranial pressure? prospective observational study employing Optic nerve sheath diameter measurements[J]. BMC Anesthesiol, 2023, 23(1): 79. DOI:10.1186/s12871-023-02037-9 |
| [48] | Lyu Y, Huang YL, Li ZY, et al. Interventions and strategies to prevent medical device-related pressure injury in adult patients: a systematic review[J]. J Clin Nurs, 2023, 32(19/20): 6863-6878. DOI:10.1111/jocn.16790 |
| [49] | Edsberg LE, Cox J, Koloms K, et al. Implementation of pressure injury prevention strategies in acute care: results from the 2018-2019 international pressure injury prevalence survey[J]. J Wound Ostomy Cont Nurs, 2022, 49(3): 211-219. DOI:10.1097/won.0000000000000878 |
| [50] | Kottner J, Cuddigan J, Carville K, et al. Prevention and treatment of pressure ulcers/injuries: The protocol for the second update of the international Clinical Practice Guideline 2019[J]. J Tissue Viability, 2019, 28(2): 51-58. DOI:10.1016/j.jtv.2019.01.001 |
| [51] | Kitayama M, Unoki T, Liu K, et al. Enteral nutrition practice in the prone position in patients with coronavirus disease 2019: an international one-day point prevalence analysis[J]. Clin Nutr ESPEN, 2024, 59: 257-263. DOI:10.1016/j.clnesp.2023.12.017 |
| [52] | Walter T, Zucman N, Mullaert J, et al. Extended prone positioning duration for COVID-19-related ARDS: benefits and detriments[J]. Crit Care, 2022, 26(1): 208. DOI:10.1186/s13054-022-04081-2 |
| [53] | Petit M, Fetita C, Gaudemer A, et al. Prone-positioning for severe acute respiratory distress syndrome requiring extracorporeal membrane oxygenation[J]. Crit Care Med, 2022, 50(2): 264-274. DOI:10.1097/ccm.0000000000005145 |
| [54] | Pan JZ, Gu M, Zhao JH, et al. Safety and efficacy of enteral nutrition during prone ventilation: a meta-analysis[J]. J Int Med Res, 2025, 53(4): 03000605251322358. DOI:10.1177/03000605251322358 |
| [55] | Zhao ML, Hou YF, Zong LW, et al. Effects of prone versus supine position during enteral nutrition on clinical outcomes and complications in mechanically ventilated patients: a systematic review and meta-analysis[J]. Front Nutr, 2026, 12: 1685664. DOI:10.3389/fnut.2025.1685664 |
| [56] | [Expert consensus on management of pain, agitation and related issues in adult patients with critical respiratory diseases]. Zhonghua Jie He He Hu Xi Za Zhi 2023, 46(12): 1162-1175. |
| [57] | Cunha PD, Barbosa TP, Correia G, et al. The ideal patient positioning in spine surgery: a preventive strategy[J]. EFORT Open Rev, 2023, 8(2): 63-72. DOI:10.1530/eor-22-0135 |
| [58] | de Miguel-Balsa E, Blasco-Ruso T, Gómez-Medrano N, et al. Effect of the duration of prone position in ARDS patients during the SARS-CoV-2 pandemic[J]. Med Intensiva Engl Ed, 2023, 47(10): 575-582. DOI:10.1016/j.medine.2023.03.011 |
 2026, Vol. 35
2026, Vol. 35